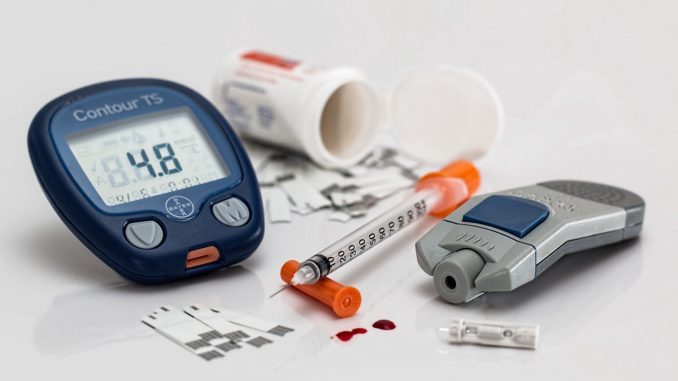
Diabetes is a disease that is on the increase worldwide. In Germany alone, more than 6 million people have diabetes – and the trend is rising. In order to avoid damage to organs and body parts in this disease, it is important to detect it early and treat it correctly.
Medical progress, with the help of digitalization, today offers many possibilities to make everyday life a little easier for diabetics.
Diabetes apps
In the meantime, there are a large number of diabetes apps that help the patients to document their daily handling of the measurement of blood sugar levels, insulin administration and the intake of carbohydrates: Electronic diabetes management instead of a handwritten diary. Most blood glucose meters today store at least the last 500 blood glucose readings with date and time. These can then be read out and processed graphically. But not all offers on the net are really recommendable. Many health apps have a decisive disadvantage: Not all apps require certification as medical devices. The user should therefore first of all make sure that the app contains the functions that meet his or her personal requirements on the one hand, and that all security-related issues are taken into account on the other. Does the app have a CE mark and does the app provider comply with all data protection regulations? Is the app regularly updated? Does it contain all the functions of an electronic diary that are helpful? Can data be automatically and securely transferred to healthcare facilities and how is the data recorded from the device or sensor into the app application?
Digital algorithms and tools – AI and Big Data
Today, the market offers a wide range of digital aids that are used to detect diabetes or to measure blood sugar levels and calculate insulin levels. One example is digital retinal screening. This is a new and promising method in the diagnosis of this disease. Based on optical coherence tomography (OCT), in which various changes in the retina and its vessels are scanned within a few seconds, it is possible to detect both existing and developing diabetes. The data from the scans are then analysed using automated algorithms by comparing them with standard values of healthy people, with deviations indicating a disease.
Another helpful innovation is, for example, the FreeStyle Libre System, which is designed to help type 1 diabetics in particular to avoid routine sugar measurements with lancing devices and test strips. With this method a sensor is attached to the back of the upper arm. The sensor now continuously measures the sugar levels and stores them automatically. A glucose meter collects the data from the outside, stores them and shows the current value and the trend in which the current sugar level is moving. A matching app is also available for the user, which can share the data obtained with the diabetes advisor or a doctor of his choice.
The insulin pump is a further aid. More than 10% of type 1 diabetics today use a pump instead of a pen to apply insulin. However, health insurance companies only cover the costs in certain cases. A distinction is made between a conventional insulin pump and an insulin patch pump. The advantage of the insulin patch pump is that it enables reliable, tubeless insulin therapy without an infusion set. The system thus consists of only two elements: the insulin patch pump (Pod), which is attached to the skin, and the management system for controlling the Pod (PDM = Personal Diabetes Manager).
One can be curious to see which new digital developments in diabetes therapy will be implemented. But one thing is clear: digitalization continues to play an important role.
© PatientCareNews.com, Author: Frank Bergs
